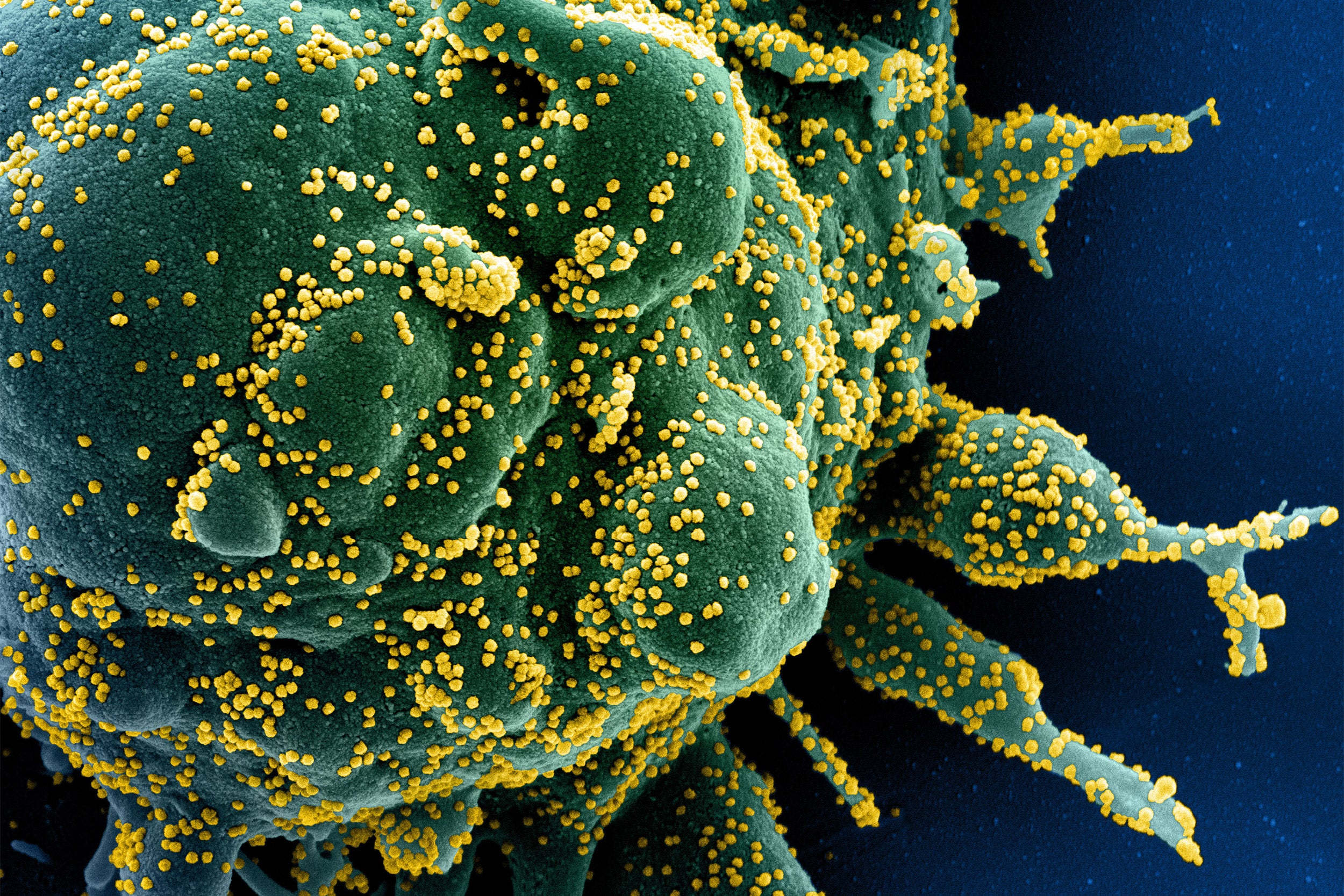
Colorized scanning electron micrograph of an apoptotic cell (green) heavily infected with SARS-CoV-2 virus particles (yellow).
Credit: NIAID
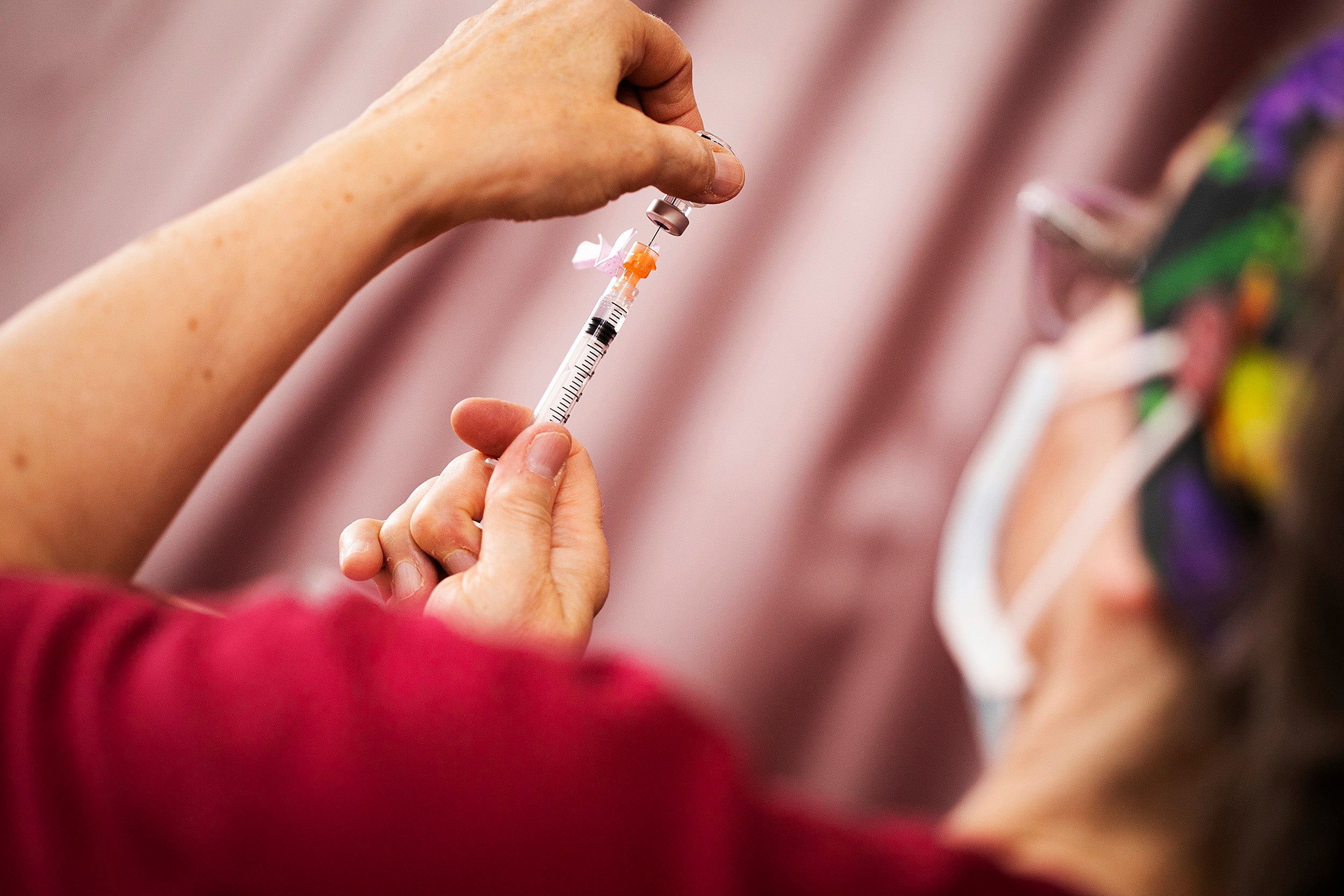
Vaccines can protect against COVID-19 in animal models, study says
Harvard-affiliated Beth Israel Deaconess Medical Center has developed vaccines — currently being tested in animal models — that are designed to train the body’s immune system to recognize the virus swiftly upon exposure and respond quickly to disable it.
This is part of our Coronavirus Update series in which Harvard specialists in epidemiology, infectious disease, economics, politics, and other disciplines offer insights into what the latest developments in the COVID-19 outbreak may bring.
With nearly 5 million confirmed cases globally and more than 300,000 deaths from COVID-19, much remains unknown about SARS-CoV-2, the virus that causes the disease. Two critical questions are whether vaccines will prevent infection with COVID-19, and whether individuals who have recovered from COVID-19 are protected against re-exposure to the virus.
Now, a pair of new studies led by researchers at Harvard-affiliated Beth Israel Deaconess Medical Center (BIDMC) suggests the answer to these questions is yes, at least in animal models. Results of these studies were published today in the journal Science.
“The global COVID-19 pandemic has made the development of a vaccine a top biomedical priority, but very little is currently known about protective immunity to the SARS-CoV-2 virus,” said senior author Dan H. Barouch, director of the Center for Virology and Vaccine Research at BIDMC. “In these two studies, we demonstrate in rhesus macaques that prototype vaccines protected against SARS-CoV-2 infection and that SARS-CoV-2 infection protected against re-exposure.”
In the first study, the team found that six candidate DNA vaccines — each formulation using a different variant of the key viral protein — induced neutralizing antibody responses and protected against SARS-CoV-2 in rhesus macaques.
Barouch and colleagues, who began working toward a COVID-19 vaccine in mid-January when Chinese scientists released the SARS-CoV-2 genome, developed a series of candidate DNA vaccines expressing variants of the spike protein, the part used by the virus to invade human cells and a key target for protective antibodies. The vaccines are designed to train the body’s immune system to recognize the virus swiftly upon exposure and respond quickly to disable it.
To assess the efficacy of the vaccines, the researchers immunized 25 adult rhesus macaques with the investigational vaccines. Ten animals received a sham version as a control group. Vaccinated animals developed neutralizing antibodies against the virus. Three weeks after a booster vaccination, all 35 animals were exposed to the virus. Follow-up testing revealed dramatically lower viral loads in vaccinated animals, compared with the control group. Eight of the 25 vaccinated animals demonstrated no detectable virus at any point following exposure to the virus, while the other animals showed low levels of virus. Moreover, animals that had higher antibody levels had lower levels of the virus, a finding that suggests neutralizing antibodies may be a reliable marker of protection and may prove useful as a benchmark in clinical testing of SARS-CoV-2 vaccines.
In the second study, the team demonstrated that macaques that recovered from COVID-19 developed natural protective immunity against re-infection with the virus. The results shed much-needed light on the critical question of just how much, if any, immunity does infection with SARS-CoV-2 provide against subsequent encounters with the virus.
“Individuals who recover from many viral infections typically develop antibodies that provide protection against re-exposure, but not all viruses generate this natural protective immunity,” said Barouch, who is also professor of medicine at Harvard Medical School, a co-leader of the vaccine development group of the Massachusetts Consortium on Pathogen Readiness, and a member of the Ragon Institute of MGH, MIT, and Harvard.
After exposing nine adult macaques to the SARS-CoV-2 virus, the researchers monitored viral levels as the animals recovered. All nine animals recovered and developed antibodies against the virus. More than a month after initial infection, the team re-exposed the rhesus macaques to the virus. Upon second exposure, the animals demonstrated near-complete protection against the virus. These data suggest that animals develop natural protective immunity against the virus and the disease that it causes.
“Our findings increase optimism that the development of COVID-19 vaccines will be possible,” said Barouch. “Further research will be needed to address the important questions about the length of protection as well as the optimal vaccine platforms for SARS-CoV-2 vaccines for humans.”
Future studies will test the Ad26 based vaccines that Barouch is developing in partnership with Johnson & Johnson.
Barouch’s co-authors included Jingyou Yu, Lisa H. Tostanosi, Lauren Peter, Noe B. Mercado, Katherine McMahan, Shant H. Mahrokhian, Joseph P. Nkolola, Jinyan Liu, Zhenfeng Li, Abishek Chandrashekar, Esther A. Bondzie, Gabriel Dagotto, Makda S. Gebre, Xuan He, Catherine Jacob-Dolan, Marinela Kirilova, Nicole Kordana, Zijin Lin, Lori F. Maxfield, Felix Nampanya, Ramy Nityanandam, John D. Ventura, Amanda J. Martinot, Lauren Peter, Peter Abbink, Michelle A. Lifton, and Huahua Wan of BIDMC; David R. Martinez and Ralph S. Baric of University of North Carolina at Chapel Hill; Carolin Loos, Caroline Atyeo, Stephanie Fischinger, John S. Burke, Aaron G. Schmidt, Galit Alter and Matthew D. Slein of Ragon Institute of MGH, MIT and Harvard; Yuezhou Chen, Adam Zuiani, Felipe J.N. Lelis, Meghan Travers, Duane R. Wesemann and Shaghayegh Habibi of Brigham and Women’s Hospital; Laurent Pessaint, Alex Van Ry, Jack Greenhouse, Tammy Taylor, Kelvin Blade, Renita Brown, Anthony Cook, Brad Finneyfrock, Alan Dodson, Elyse Teow, Hanne Anderson, Mark G. Lewis and Jason Velasco of Bioqual; Roland Zahn and Frank Wegmann of Janssen Vaccines and Prevention BV; Yongfei Cai and Bing Chen of Children’s Hospital Boston; Zoltan Maliga and Peter K. Sorger of Harvard Medical School; Michael Nekorchuk, Kathleen Busman-Sahay, Margaret Terry and Jacob D. Estes of Oregon Health &Science University; LindaM. Wrijil and Sarah Ducat of Tufts University Cummings School of Veterinary Medicine; and Andrew D. Miller of Cornell University College of Veterinary Medicine.
The authors declare no competing financial interests.
These studies were supported by the Ragon Institute of MGH, MIT, and Harvard; Mark and Lisa Schwartz Foundation; Beth Israel Deaconess Medical Center; Massachusetts Consortium on Pathogen Readiness; Bill & Melinda Gates Foundation; Janssen Vaccines & Prevention BV; the National Institutes of Health (grants OD024917, AI129797, AI124377, AI128751, AI126603 to D.H.B.; AI135098 to A.J.M.; AI007387 to L.H.T.; AI007151 to D.R.M.; AI146779 to A.G.S.; 272201700036I-0- 759301900131-1, AI100625, AI110700, AI132178, AI149644, AI108197 to R.S.B.; CA225088 to P.K.S.;OD011092, OD025002 to J.D.E.; and AI121394, AI139538 to D.R.W.; Burroughs Wellcome Fund Postdoctoral Enrichment Program Award; Fast Grant, Emergent Ventures, Mercatus Center at George Mason University.