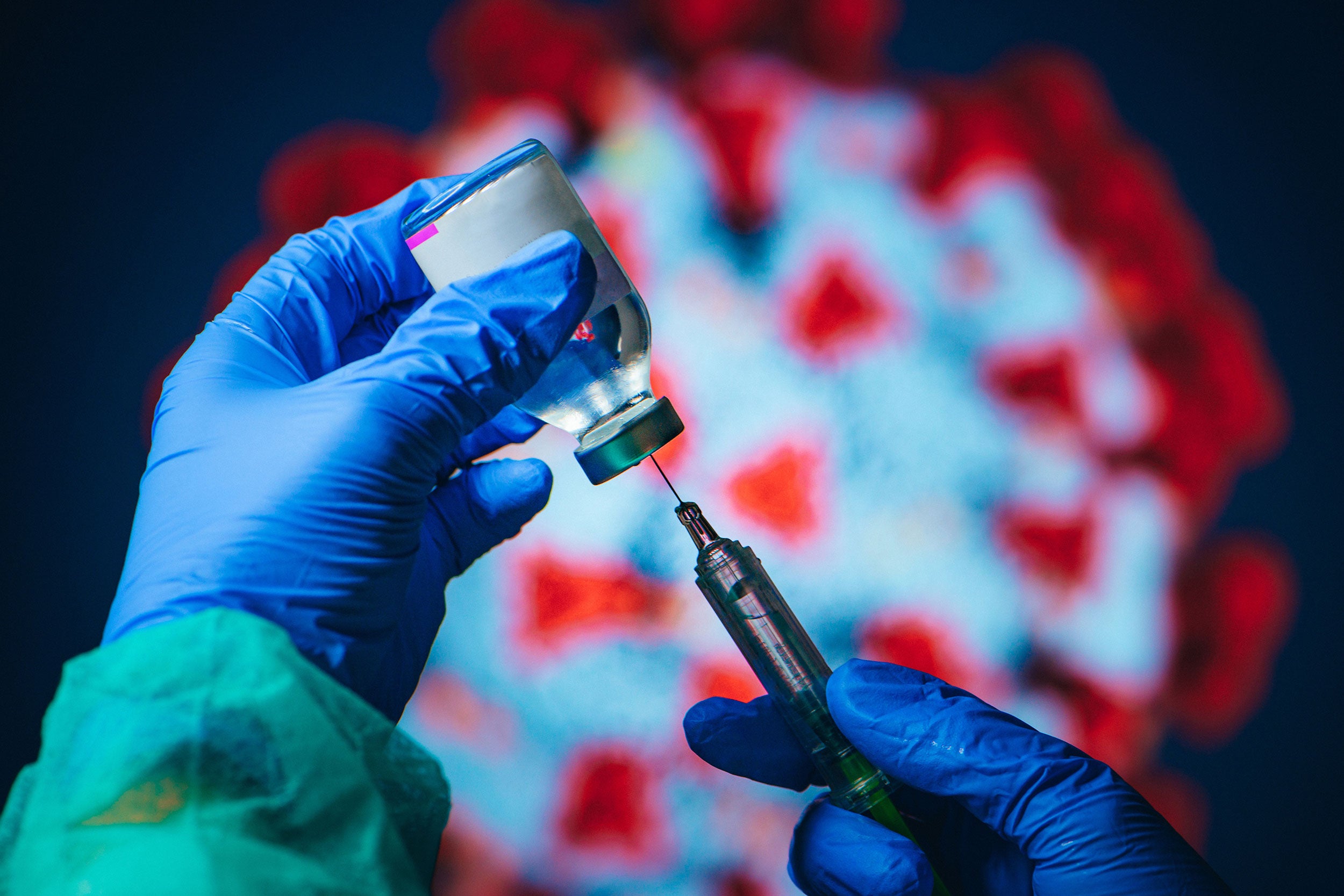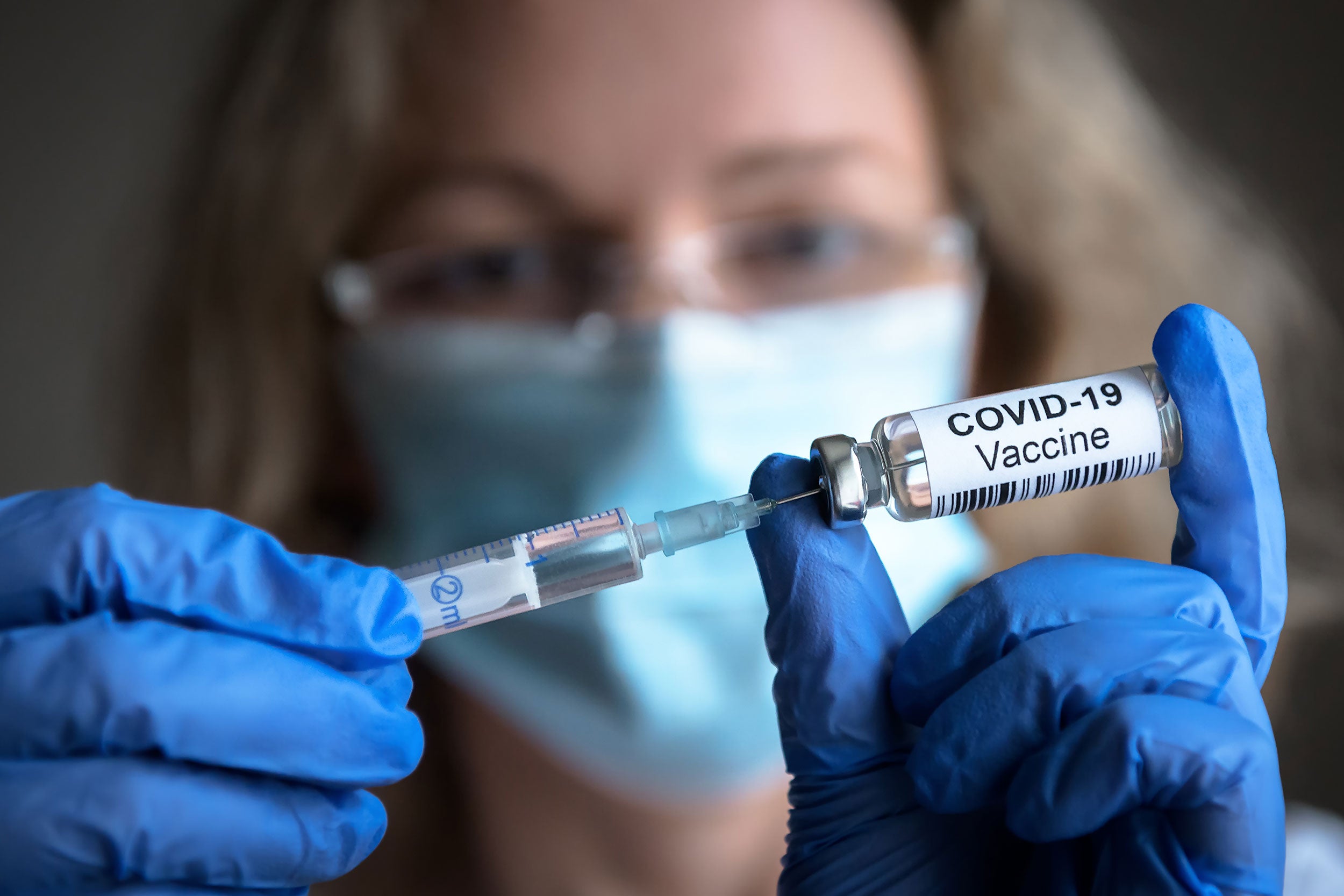
Over a three-day period following their COVID-19 vaccine, hospital employees were asked to use a decision-support tool, which asked a series of questions to determine if their symptoms were vaccine or virus related.
Scaliger/iStock
Researchers’ tool discerns COVID symptoms from vaccine reaction
A new decision-support tool helped preserve the health care workforce by distinguishing symptoms associated with COVID-19 vaccinations from symptoms of the virus itself.
A decision-support tool helped health care workers distinguish symptoms associated with COVID-19 vaccinations from symptoms of the virus itself, found a study by investigators from Harvard-affiliated hospitals in the Massachusetts General Brigham system.
The study , published in Infection Control & Hospital Epidemiology, suggests that providing this guidance may keep employees from needlessly missing work during a critical time and help curb the spread of COVID-19 in health care settings. The study assessed employees vaccinated from Dec. 16, 2020 to March 14, 2021, in the midst of a sharp increase of COVID-19 cases in the United States, including Massachusetts.
“That’s also when we were vaccinating tens of thousands of employees, all in a very short period of time,” says the study’s co-lead author, infectious diseases specialist and health care epidemiologist Erica S. Shenoy, associate chief of the Infection Control Unit at Massachusetts General Hospital and associate professor of medicine at Harvard Medical School.
Shenoy and her colleagues recognized a potential problem with the massive number of MGB employees getting the vaccines over a short period. In keeping with public health requirements, employees at all MGB facilities must attest that they are not experiencing any symptoms of COVID-19 before reporting to work each day. However, receiving a COVID-19 vaccination can trigger a variety of symptoms, and some overlap with those caused by the virus itself, including fever, fatigue, and muscle or joint pain. That meant that a large number of MGB employees could fail attestation in the first few days after getting vaccinated and miss work, even though the symptoms that kept them home were more likely related to receiving the vaccine than to COVID-19.
“Workforce preservation was critically important,” says Shenoy. “We were in the middle of another surge and we had to make sure everyone who could be at work could do so safely.”
Shenoy and her colleagues developed an electronic decision-support tool for smartphone or computer that MGB employees were asked to use during the three days after vaccination. The tool presented a list of symptoms, some associated with allergic reactions (such as a rash or wheezing), others with COVID-19 (such as cough, nasal congestion, and loss of taste or smell), and still other symptoms that overlapped between the two. The user checked off any they were experiencing and was asked to rate the symptoms’ severity (severe or mild/moderate). Based on their answers, users were advised whether they could report to work or should stay home and get tested for COVID-19. Those who reported mild vaccine-related symptoms were advised on how to treat them.
Participation by MGB employees was exceptional, with 83 percent responding after getting their first dose of either the Pfizer-BioNTech or Moderna vaccine, while 77 percent responded after their second dose. (The Johnson & Johnson/Janssen vaccine was excluded from the study because it wasn’t introduced in the United States until early March.) The portion of participants who tested positive for COVID-19 was very low. Positive cases were more likely to be detected in participants who had three or more low-severity overlap symptoms, one or more high-severity overlap symptoms, or at least one typical COVID-19 symptom such as cough or runny nose. Interestingly, employees who had a COVID-19 infection prior to getting vaccinated were significantly more likely to report severe overlap symptoms after their first dose, though it’s not clear why.
“This paper speaks to the importance of having a system in place that provides guidance to a workforce being vaccinated around the confusing questions of when to come to work, when to pursue testing, and how to treat milder symptoms,” says co-first author Paige Wickner, who serves on the faculty in the Division of Allergy and Clinical Immunology at Brigham and Women’s Hospital and is an assistant professor at HMS. Without offering vaccinated employees a framework for making these decisions, says Wickner, “you risk losing a lot of staff at a critical time. This study is an exciting first step toward providing that guidance, which will be critical in the coming months and years.” To wit: Shenoy, Wickner, and their colleagues are currently collecting similar data from MGB employees who are receiving COVID-19 booster shots.
This work was supported by the Roger I. and Ruth B. MacFarlane Foundation, Harvard Catalyst, the Harvard Clinical and Translational Science Center, and financial contributions from Harvard University and its affiliated academic health care centers.